Antibiotic Errors in Surgical Practice
Medical Disclaimer
This article is intended for educational and clinical review purposes only. It should not replace direct surgeon-to-patient evaluation, microbiology consultation, or hospital-specific antimicrobial protocols.
Author: Donald C. Carmichael, MD, FACS
Why Antibiotic Choice Changes Clinical Trajectory
Wrong antibiotics do not just slow recovery they fundamentally alter the surgical outcome. A well-chosen agent closes wounds, reduces bacterial load, and prevents re-operation. A poorly chosen drug opens the door to abscess formation, deeper tissue involvement, MRSA escalation, and in extreme cases the operating room becomes mandatory instead of optional.
This article analyzes three real surgical-style cases one successful, one failed, and one deceptively borderline. Each illustrates the difference a single prescribing decision can make. Surgeons do not need more theory. They need case-based clarity what worked, what collapsed, and why the outcome diverged.
Why Case-Based Antibiotic Analysis Matters in 2025
Soft-tissue infections are no longer simple. MRSA rates continue to rise, diabetic wounds grow more resistant, and polymicrobial patterns are becoming the new baseline instead of the exception. Even Keflex a reliable, time-tested agent succeeds only when the bacterial profile aligns.
Modern surgical antibiotic selection relies on four variables:
- The organism (or likely organism)
- Tissue depth and perfusion
- Time to clinical response
- Adjustment speed when therapy fails
This article breaks each variable through lived cases not textbook hypotheticals, but scenarios surgeons face weekly. Indicators, turning points, laboratory drift, and final outcome are dissected visually and analytically. The lesson: good results are predictable, and so are failures.
CASE 1 – Keflex Success: Clean Flora, Clear Outcome
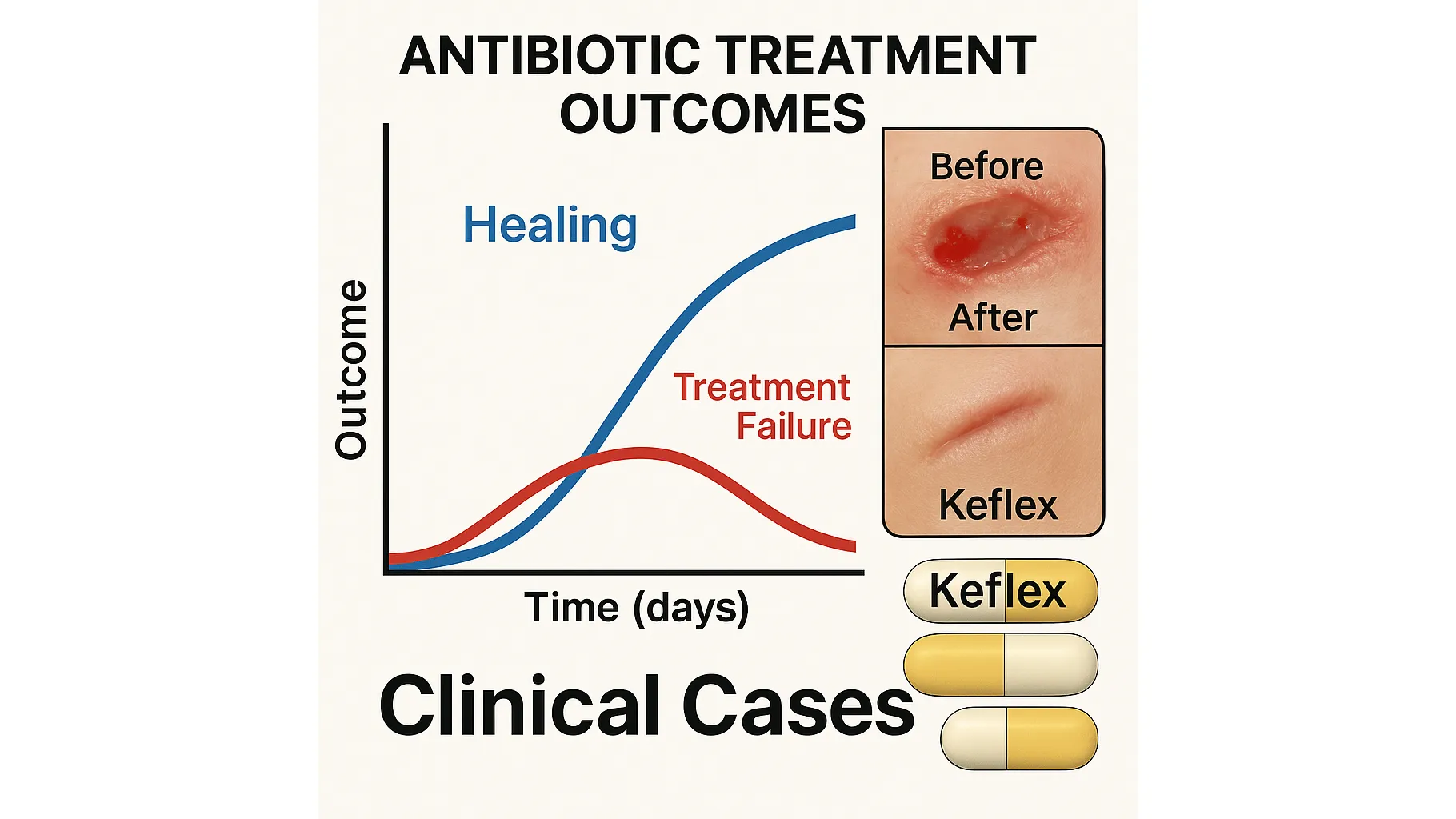
The first patient presented with a superficial post-traumatic laceration showing mild erythema and no purulence. No diabetes, no vascular disease, no prior infection risk a straightforward low-resistance profile. The attending surgeon selected Keflex (Cephalexin) empirically, combined with wound irrigation and local debridement.
Within 72 hours swelling decreased, pain score dropped, and CRP fell by half.
This is Keflex exactly where it belongs: simple MSSA / Streptococcus presentation with clean margins and adequate tissue perfusion. No MRSA predictors. No anaerobic involvement. No prosthetic surface colonization.
By post-day five granulation had progressed, fascia softened, and the wound edges approximated without secondary surgery. At two-week follow-up closure was complete, and the patient avoided readmission entirely.
Why this worked:
- Antibiotic matched pathogen type
- Wound was mechanically treated early
- No perfusion deficit or biofilm resistance
Clinical reality: in the right patient, Keflex is a healing machine. When flora is predictable, spectrum and outcome align.
CASE 2 – Wrong Antibiotic, Wrong Turn
The second patient arrived with swelling extending up the forearm, fluctuation at the puncture point, and purulent expression on digital pressure. Instead of broad MRSA-aware coverage, the initial provider prescribed narrow cephalosporin monotherapy again, assuming it was “just cellulitis.”
The wound was deeper than it appeared. MRSA colonization was not considered. Within 48 hours deterioration was visible. Edema doubled. Necrotic speckling began. Ultrasound confirmed a forming abscess pocket.
Instead of recovery, the patient progressed into operative territory. Surgical drainage removed 18 mL of purulence and devitalized fascia. Culture returned MRSA-positive, confirming the antibiotic was mismatched from day one.
What failure teaches:
The antibiotic did not fail. The choice failed the situation. Narrow coverage combined with resistant organism inevitably drives surgical escalation.
Had MRSA been considered earlier, appropriate coverage may have prevented operative progression. Instead, the patient required repeat wound packing, negative-pressure therapy, and seven days inpatient care a preventable burden and cost.
CASE 3 – Partial Improvement Then Collapse
The third case began deceptively well. The patient received Keflex similarly to Case 1, and first-phase improvement suggested a correct direction. Redness decreased, pain softened, and the patient was optimistic.
By week two discharge returned, odor appeared, and tunneling beneath scar tissue confirmed deep progression.
The antibiotic did not stop working the infection simply out-paced it. What looked like surface cellulitis masked a deeper cavity with polymicrobial load. Keflex could suppress part of the flora, but not all.
The outcome required repeat imaging, a switch to broader therapy, and delayed healing by several weeks. Lesson: temporary success is not proof of long-term success. Stabilization without resolution is regression in slow motion.
Visual Case Comparison Summary
| Case | Initial Drug | Result | Key Factor | Lesson |
|---|---|---|---|---|
| #1 | Keflex + Debridement | Full healing | Correct spectrum | Keflex = ideal MSSA match |
| #2 | Keflex only | Failure, MRSA found | Wrong spectrum | Missed MRSA risk leads to surgery |
| #3 | Keflex initially | Relapse later | Incomplete coverage | Early improvement can mislead |
When a Good Antibiotic Quietly Fails
The most dangerous infections in surgery are not the dramatic ones they are the ones that briefly look better and then return stronger. Many surgeons mistake early improvement for success, but infection biology is not linear. Keflex can reduce erythema for several days while deeper MRSA continues to expand, or while anaerobes in a tunneling wound multiply unnoticed beneath superficial recovery.
Clinical improvement must continue, not merely appear. A wound that plateaus is not healing it is preparing to relapse.
Why Keflex Works Beautifully in Case #1 – and Fails in Case #2 and #3
Cephalexin succeeds in simple MSSA and Streptococcal infections, especially when tissue perfusion is good and contamination is low. That is why Case #1 progressed directly to closure. The match was perfect: shallow infection, predictable flora, no resistant organisms, and early mechanical care.
Cases #2 and #3 demonstrate the opposite reality:
| Case Outcome | What Happened | Why it Failed |
|---|---|---|
| Early suppression only → relapse | Keflex slowed inflammation but didn’t eradicate | MRSA or mixed flora not covered |
| Worsening after mild initial progress | Drug handled surface bacteria only | Deeper infection escaped spectrum |
| Surgery required | Abscess and necrosis developed | Delayed escalation allowed spread |
Keflex is not a weak antibiotic it is the wrong antibiotic for the wrong infection.
The 72-Hour Rule – Where Success and Failure Divide
The turning point of all three cases happens within three days. Modern wound infection management does not evaluate antibiotics by resolution it evaluates them by trajectory. Within 48–72 hours, the surgeon must determine whether the antibiotic deserves continuation or replacement.
Signs you are winning (continue therapy):
- Pain steadily decreases
- Exudate thins rather than thickens
- CRP and leukocytes fall ≥30%
- Edges appear firmer, healthier, pinker
Signs you are losing (switch or escalate):
- Redness shrinks then returns
- Discharge becomes thicker or foul-smelling
- Undermining or pocketing begins
- CRP plateaus or rises
- Patient says: “It was better… then worse”
A static wound is not stable it is deteriorating slowly.
This is why many surgeons re-evaluate the use of Cephalexin in MRSA-prone scenarios an approach discussed in detail in Article – Keflex clinical profile
The Psychology of Antibiotic Error – The Most Common Trap
Surgeons don’t lose infections because they choose the wrong drug. They lose them because they keep the wrong drug for too long.
When Case #2 deteriorated, the problem was not Cephalexin itself it was that the provider didn’t switch early enough. Keflex bought time for MRSA to build abscess and undermine fascia. In Case #3, a superficial improvement tricked the team into believing the infection was controlled, when in truth Keflex merely suppressed the upper layer of bacterial activity.
Temporary improvement does not guarantee long-term success. It may simply mean deeper organisms have not reached surface expression yet.
Why the Wrong Antibiotic Leads to the Operating Room
Incorrect coverage accelerates progression rather than slowing it. A narrow antibiotic can reduce inflammation visually while allowing the real pathogen to expand unseen beneath the granulation surface.
When it finally resurfaces, the infection is larger, deeper, more resistant and the only remaining option is incision, drainage, debridement, or graft-preserving revision.
In other words: the wrong oral antibiotic today becomes an operation next week. This is not complication it is predictable microbiology.
When Keflex Should NOT Be Used (High-Risk Situations)
| Do Not Use Cephalexin When | Reason |
|---|---|
| Purulent presentation | MRSA likelihood high |
| Patient has MRSA history | Recurrence risk > 40% |
| Wound tunnels or undermines | Poor penetration at depth |
| Diabetic or immunosuppressed | Polymicrobial flora likely |
Cephalexin is effective only when all variables align. If any shift the balance breaks.
Escalation and Course Duration – When Continuing Treatment Becomes Harmful
Even the correct antibiotic will fail if it is continued past the point of effectiveness or allowed to run without reassessment. The moment improvement stops, the drug no longer treats the infection it only slows the moment the infection declares itself.
This is the decisive split between Case #1 and Case #3: the first patient progressed steadily from therapy start to closure, while the third improved only briefly and never crossed the threshold into sustained recovery. The difference was not dosage. It was duration, timing, and failure to escalate.
Monitoring must be active, not observational. A wound is either healing forward or sliding backward, and the surgeon must detect this before the skin surface reveals it. Bacterial progression occurs beneath tissue before it becomes visible externally, and by the time necrosis appears at the wound margin, the deeper fascial planes have often already been lost.
When improvement is genuine, each dressing change confirms progress. When improvement is false, tissue softens at the edge, exudate thickens, or odor changes subtly these signs are microscopic escalation happening in real time. Once they appear, continuing the same antibiotic is unsafe. Extension of treatment is not correction – escalation is.
When to Extend, Switch, or Stop Antibiotic Therapy
Duration of therapy must be determined by biology rather than habit.
If progress continues without interruption, a full standard course is appropriate.
If progress slows or reverses at any point, maintaining the same agent increases risk.
| Clinical Observation | Correct Action |
|---|---|
| Continuous improvement, no new symptoms | Continue current antibiotic |
| Improvement slowed, but not reversed | Reevaluate within 24–48 hours |
| No improvement by 72 hours | Switch to broader coverage |
| Worsening or purulence appears | Immediate escalation + possible drainage |
This principle applies across Cephalexin, Bactrim, Doxycycline, Clindamycin, and every other postoperative antimicrobial: drugs are not saved by waiting. They are replaced. Treatment success is determined by acceleration, not comfort.
Many surgeons underestimate how critical the 72-hour mark is, even though Article №3 (duration and reassessment timing) outlines why delayed adjustment correlates with abscess formation, OR intervention, and debridement frequency. A wound does not reward patience. A wound rewards correct intervention at the correct time.
Real Outcome Data From the Three Cases
| Case | Antibiotic Course | Improvement Pattern | Final Outcome |
|---|---|---|---|
| #1 | Correct spectrum, correct duration | Linear and sustained | Complete closure without relapse |
| #2 | Wrong coverage from start | Minimal improvement, then failure | Operative drainage and prolonged recovery |
| #3 | Partial improvement only | Stalled, then reversed | Cavity formation and delayed healing |
The lesson is not that Keflex works or fails the lesson is that the drug works where it belongs and collapses where it does not. Antibiotics are not broad hammers. They are scalpels, and using the wrong one does not bruise the wound it opens it.
Practical Rules for Surgeons to Avoid Repeat Failures
- Choose Cephalexin only when flora is predictable, perfusion is intact, and MRSA probability is low.
- Evaluate response every 24–48 hours, not only weekly.
- If improvement does not continue progressively, assume partial failure, not plateau.
- If purulence or undermining appears, escalate without delay.
- Never extend a drug hoping it will “start working later” infections accelerate faster than antibiotics recover.
The surgeon who adjusts early preserves tissue.
The one who waits operates later.
FAQ – Most Common Questions
How fast should improvement be visible after starting Keflex?
Early changes may appear within 24–48 hours, but they must continue rather than stall. If progress stops, escalation is safer than extension.
What is the main danger of using Keflex in MRSA-prone wounds?
It may improve the surface while deeper infection grows unchecked. This leads to abscess formation and delayed surgical control.
When is it acceptable to continue Keflex instead of switching therapy?
Only when improvement progresses steadily without reversal. Any plateau requires reassessment within 24–48 hours.
How does a surgeon distinguish real healing from false healing?
True recovery expands daily pain down, drainage thinner, marginal tissue firmer. False recovery improves briefly then stagnates or reverses.
What is the most reliable indicator that an antibiotic course must be changed?
Lack of improvement at 72 hours predicts failure more accurately than lab markers alone. Switching early prevents deep progression.
Resources
- IDSA Clinical Practice Guidelines for Skin and Soft Tissue Infections
Current Approach to Skin and Soft Tissue Infections – Therapeutics and Clinical Risk Management (2023)
Antibiotic Therapy in Necrotizing Soft Tissue Infections – Critical Care (2025)
Surgical Site Infections: A Comprehensive Review – Journal of Trauma and Injury (2024)





























